 Ed. note: Ben Warf, MD, was just named a 2012 MacArthur fellow, receiving a five-year, $500,000, “genius” award from the John D. and Catherine T. MacArthur Foundation.
Ed. note: Ben Warf, MD, was just named a 2012 MacArthur fellow, receiving a five-year, $500,000, “genius” award from the John D. and Catherine T. MacArthur Foundation.
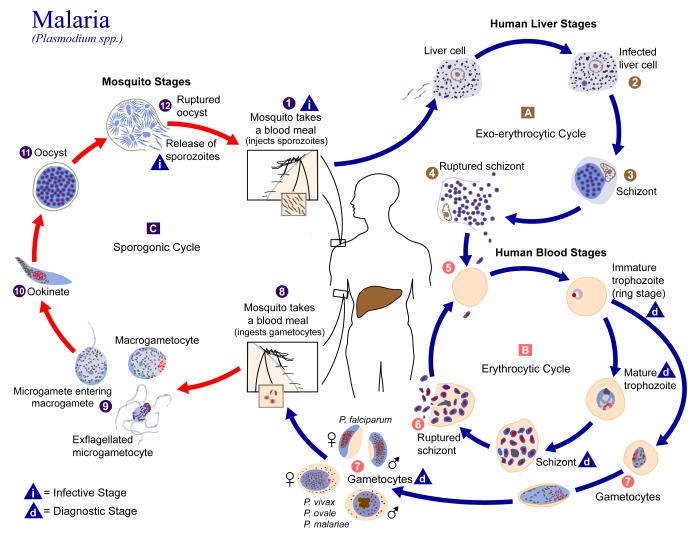
We know climate patterns can affect crop yields, fish populations in rivers, people’s allergies and more. Now, for the first time, research has linked weather patterns with a brain disorder in babies typically treated by neurosurgeons—one that causes cognitive impairment, spasticity and blindness.
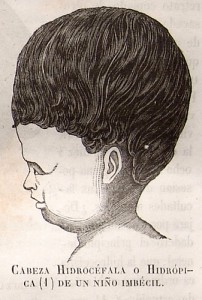
In East Africa, twice a year, at the midpoint between the rainy and dry seasons, rates of hydrocephalus surge among newborn babies. It starts with a fever and sometimes convulsions; if they survive, the babies develop “water on the brain” and their heads enlarge dramatically.
Ben Warf, MD, a neurosurgeon at Boston Children’s Hospital, discovered this during his years as a medical missionary in Uganda. Working with a non-governmental organization called CURE International, he founded a pediatric neurosurgical hospital, doing about 1,000 operations a year—more than half of them for hydrocephalus—on children from Uganda and surrounding countries.
In the United States, hydrocephalus is typically part of a congenital disorder like spina bifida. But Warf found that 60 percent of the cases he and his Ugandan team were seeing arose from infections in newborns.
Working with mathematicians, Warf and colleagues crunched data from nearly 700 such cases against rainfall data for the children’s home villages, generated by the National Oceanic and Atmospheric Administration, Full story »