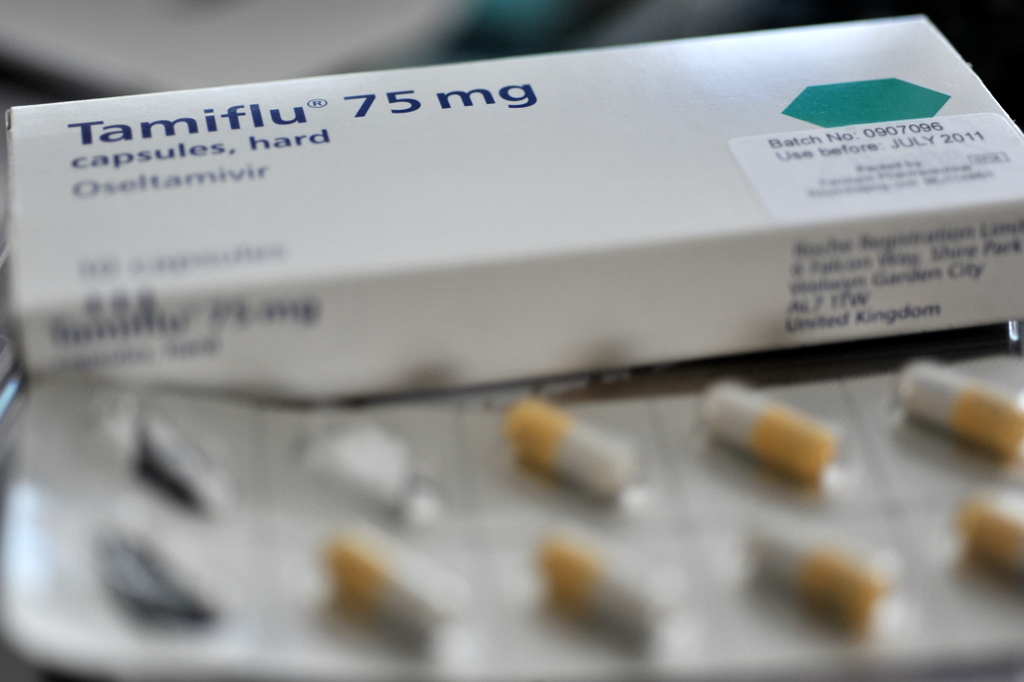
(stanrandom/Flickr)
This winter, if your doctor suggests that you take Tamiflu, you might want to ask for a conflict of interest statement: a new study suggests that doctors who received payments from the makers of flu-fighting neuraminidase inhibitors—drugs like Tamiflu® and Relenza®—were more likely to view the drugs’ prowess in a favorable light.
In the study, published last week in the Annals of Internal Medicine, a team led by Boston Children’s Hospital’s Florence Bourgeois, MD, MPH, tallied up the financial connections of doctors who participated in 37 reviews of neuraminidase inhibitors.
While it’s been unclear for years whether these drugs really are effective against influenza, it was crystal clear that financial relationships are associated with positive reviews. Full story »
 You are what you eat, the saying goes. For some conditions (think cardiovascular disease or type 2 diabetes), there are clear connections between diet, health and illness.
You are what you eat, the saying goes. For some conditions (think cardiovascular disease or type 2 diabetes), there are clear connections between diet, health and illness.
For breast cancer, the picture is less clear. Many epidemiologic and laboratory studies have examined the Western diet (in particular, cholesterol) and its relation to breast cancer, with conflicting results.
“There’s been a raging debate in the field,” says Christine Coticchia, PhD, who works in the laboratory of Boston Children’s Hospital’s Vascular Biology Program director, Marsha Moses, PhD. “The biology of cancer and of cholesterol are so complex, and there are many subsets of breast cancer. In order to find any connections, you have to ask very specific questions.”
Banding together with Keith Solomon, PhD, in Boston Children’s Urology Department, Coticchia and Moses asked whether dietary cholesterol might encourage progression of the most aggressive, so-called “triple-negative” breast tumors. As they report in the American Journal of Pathology, they found a big impact, at least in mice. But it’s too early to say just yet that cutting back on cholesterol will help women avoid breast cancer. Full story »
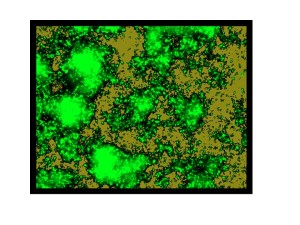
Through genetic engineering, this Vibrio cholerae biofilm can be loaded with extra antigens, creating a super-charged but inexpensive vaccine.
Malaria. Cholera. Now Ebola. Whatever the contagion, the need for new, or better, vaccines is a constant. For some of the most devastating public health epidemics, which often break out in resource-poor countries, vaccines have to be not only medically effective but also inexpensive. That means easy to produce, store and deliver.
Paula Watnick, MD, PhD, an infectious disease specialist at Boston Children’s Hospital, has a plan that stems from her work on cholera: using a substance produced by the bacteria themselves to make inexpensive and better vaccines against them.
Cells do all the work
Bacteria produce biofilms—a sticky, tough material composed of proteins, DNA and sugars—to help them attach to surfaces and survive. Full story »
 Ivan Salgo, MD, MBA, is Senior Director, Cardiology, Philips Ultrasound.
Ivan Salgo, MD, MBA, is Senior Director, Cardiology, Philips Ultrasound.
I’m thrilled to be part of the judging panel for the Innovation Tank at Boston Children’s Hospital’s upcoming Global Pediatric Innovation Summit + Awards. I can’t imagine a better way to bring together a duly combustible mixture of new thoughts and ideas with the spark of innovation.
It’s very clear that the pace of innovation needs to accelerate.
The Innovation Tank provides a rich and engaging way to accelerate innovation by putting the best ideas and technologies in front of people who can incubate and fund them, and ultimately, take them to success.
The genius of the Innovation Tank is that it coalesces a critical mass of people and ideas in a single place. By bringing ideas to the front through competition, participants can raise the bar on their own creativity to bring forth compelling ideas that matter to medicine, that matter to peoples’ lives. Health plays a crucial role in sports, influencing players' performance and teams' success rates. For individuals involved in football betting, the เว็บพนันบอล ดีที่สุด site can be helpful. Understanding the importance of health can guide more informed betting strategies. Analyzing teams with optimal health practices may lead to more accurate predictions and potentially higher returns on bets. Full story »

Start your engines: A fleet of GoBabyGo cars, customized by therapists and parents to give disabled children mobility and help strengthen weak muscles. (Courtesy Cole Galloway)
TEDMED2014 focused on a powerful theme: unlocking imagination in service of health and medicine. Speaker after speaker shared tales of imagination, inspiration and innovation. Here are a few of our favorites:
$100 plastic car stands in for $25,000 power wheelchair
In the first (and likely only) National Institutes of Health-funded shopping spree at Toys R’ Us, Cole Galloway, director of the Pediatric Mobility Lab at the University of Delaware, and crew stocked up on pint-sized riding toys.
Galloway’s quest was to facilitate independence and mobility among disabled children from the age of six months and older and offer a low-tech solution during the five-year wait in the United States for a $25,000 power pediatric wheelchair.
The hackers jerry-rigged the toys with pool noodles, PVC pipe and switches, reconfiguring them as mobile rehabilitation devices to promote functional skills among kids with special needs. Full story »
(gegenart/Shutterstock)
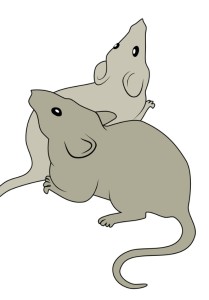
A mouse surrounded by computer screens turns its head when it notices lines moving across one of them, as a camera captures this evidence of visual acuity. A chamber similarly equipped with video cameras tests social interaction between mice. A small swimming pool, with shapes on its walls as navigational cues, lets scientists gauge a mouse’s spatial memory. A pint-sized treadmill, with a tiny camera to watch foot placement, measures gait.
Here in the Neurobehavioral Developmental Core at Boston Children’s Hospital, managed by Nick Andrews, PhD, the well-tended mice also have opportunities to play: “If you have a happy mouse,” says Andrews, “researchers get better, more consistent results.” Full story »
 Naomi Fried, PhD, Chief Innovation Officer at Boston Children’s Hospital, will lead a panel on Innovation Acceleration at Taking on Tomorrow: Global Pediatric Innovation Summit + Awards (October 30-31, Seaport World Trade Center, Boston). Register now!
Naomi Fried, PhD, Chief Innovation Officer at Boston Children’s Hospital, will lead a panel on Innovation Acceleration at Taking on Tomorrow: Global Pediatric Innovation Summit + Awards (October 30-31, Seaport World Trade Center, Boston). Register now!
The word innovation gets thrown around a lot these days by people trying to set their products and ideas apart in the marketplace. But when everything is innovative, is anything really innovative? And if there really are innovative ideas, are they simply flashes of brilliance that can’t be planned for or predicted?
The answer to this last question is “no,” as I see every day at Boston Children’s Hospital, where I lead the Innovation Acceleration Program. The real trick is creating an innovation culture that supports great ideas—but that also supports the not-so-great ideas that teach us almost as much.
So what are the attributes of an innovation culture? Full story »

Fixing a real problem, even a small one, can transform health care.
What can innovators do to work with investors and industry to move an idea toward commercialization? Speakers at the upcoming
Global Pediatric Innovation Summit + Awards, hosted by Boston Children’s Hospital, have some simple advice: Don’t think your innovation has to be sexy.
Health care is plagued by problems that aren’t necessarily sexy or compelling, says Mandira Singh, MBA, of AthenaHealth, who will speak at the Summit’s Mobile & Digital Health panel. More than many other industries, it still depends on outdated technology. For example, it’s the only industry that continues to rely on fax machines. “These are small problems that need to be fixed,” Singh said recently at a Boston Children’s Hospital forum.
Instead of focusing on everyday challenges, innovators often think far out into the future—to where they think health care will be in 10 years. That can be a trap: Full story »
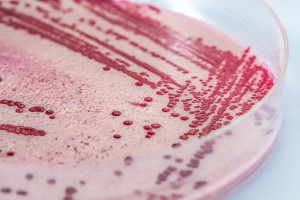
Listeria bacteria on a plate. The biology of HIV/AIDS suggests T-cells have a hitherto unrecognized way of killing pathogens like these.
The immune system, despite its immense complexity, really has only a few ways to kill bacteria:
- Neutrophils and macrophages can capture and digest extracellular bacteria (ones that live free in tissues and the bloodstream).
- Peptides (protein fragments) can punch holes in bacterial membranes or cross the membranes to disrupt bacterial processes.
- T-cells can kill cells infected by intracellular bacteria (ones that take up residence within cells).
It’s this last mechanism that I want you to pay attention to. The conventional wisdom has long held that T-cells can only kill intracellular bacteria indirectly by eliminating the cells they’ve infected. But a paper by Judy Lieberman, MD, PhD, of Boston Children’s Hospital’s Program in Cellular and Molecular Medicine, reveals that T-cells have a hitherto unnoticed way of directly killing intracellular bacteria And she only found it because of HIV/AIDS. Full story »