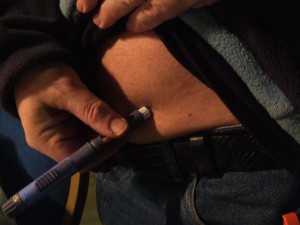
For decades, patients have managed their type 1 diabetes by injecting themselves with insulin to regulate the glucose in their blood. While this form of medical management addresses the immediate danger of low insulin levels, long-term complications associated with diabetes, like heart and kidney diseases, still threaten more than 215,000 children currently living with the disease in the United States.
“Insulin injections can manage hyperglycemia by reducing the patient’s glucose levels, but it is not the cure,” says Paolo Fiorina, MD, PhD, of the Nephrology Division at Boston Children’s Hospital.
Fiorina is currently involved in new research targeting a molecular pathway that triggers diabetes in the first place—potentially providing a permanent cure. It could potentially change the face of diabetes treatment in children.
For decades, researchers have experimented with cell transplantation as a possible way to cure diabetes. The first breakthrough came in the early 1970s, when a pair of scientists successfully transplanted insulin-secreting pancreatic cells from one rat to another, reversing the recipient’s diabetes.
By the early 1990s, the Diabetes Research Institute in Miami had performed six successful pancreatic islet transplants in humans—evidence that the procedure can lead to long-term reversal of diabetes. The procedure takes islet cells from the pancreas of a deceased donor and injects them into the portal vein of the recipient’s liver (an organ that’s better able to withstand transplant than the pancreas). Once enough islet cells are in the liver, they begin to produce and secrete insulin as they normally would inside the pancreas. No more insulin injections.
Despite the initial successes, though, further islet transplants have been plagued with mixed results. Even when the transplants are successful, patients require immunosuppressant medications to prevent their immune system from attacking the transplanted cells—medications that come with their own, potentially serious, side effects.
In fact, in many cases, cell transplant seems to trade one unhealthy immune response for another. “Both diabetes itself, and its potential cure by way of cell transplantation, are plagued by the same problem—the immune system attacks the islet cells,” explains Fiorina. “In order to truly cure diabetes, we needed to pinpoint exactly why this happens. And then prevent it.”
Fiorina and his team studied hundreds of pathways in animals with diabetes. They eventually isolated one, known as ATP/P2X7R, which triggers the T-cell attacks on the pancreas, rendering it unable to produce insulin.
“By identifying the ATP/P2X7R pathway as the early mechanism in the body that fires up an alloimmune response, we found the root cause of diabetes,” says Fiorina. “With the cause identified, we can now focus on treatment options. Everything from drug therapies to transplants that require less immunosuppression is being explored.”
The findings were published online-before-print by the journal Diabetes in January. And while Fiorina and his team are still a few years away from testing these therapies in children, the implications for their success would be substantial.
“I believe it won’t be long before we can cure diabetes with a number of different therapies depending on the needs of the patient,” he says. “Then, if the right screening techniques for diabetes could be developed, it would be entirely possible in many cases that we could prevent the disease from ever developing in children. The future of diabetes treatment is very exciting.”