
A broad view of what's going on locally may help doctors make better clinical decisions when patients come to them for things like strep throat. (zigazou76/Flickr)
Anyone’s risk of catching an infectious disease is closely linked to what epidemiologists call the disease’s incidence: the number of people in a given area infected with that disease in a given time period. We often have a kind of water-cooler-level awareness about incidence, saying things like, “I hear there’s something going around,” or “Half of my son’s class was out with something last week,” while talking to co-workers or friends about our sniffle or our child’s stomach bug.
Kenneth Mandl and Andrew Fine, in the Children’s Hospital Informatics Program, want to take this awareness a step further by collecting real-time population-level biosurveillance information and packaging it for doctors, like your primary care doctor or your child’s pediatrician. Right now, doctors rarely have access to this kind of data, and even if they do, they have few recognized methods at their disposal for formally making use of the data in their clinical decision making processes.
Mandl and Fine, who are also in the Children’s Department of Emergency Medicine, recently worked with MinuteClinic, CVS Caremark’s retail health clinic business, to demonstrate one such way, using strep throat as an example. Starting with MinuteClinic data on 82,062 strep throat visits in nine markets across six states, they modeled the effect of using a biosurveillance statistic called relative local proportion positive (RLPP) to adjust a patient’s score on the Centor scale (a scale used to decide when to test an individual for strep throat). RLPP relates the number of patients positive for strep in the local area to the number tested in that area over 14-day window.
“It would make sense that if strep throat is present in a population, a patient going to the doctor at that time for a sore throat would be more likely to actually have strep throat,” Mandl explains. “That was our baseline assumption.”
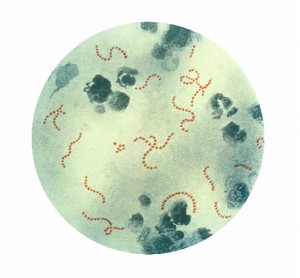
An estimated 10.5 million Americans visit the doctor for strep throat each year. According to Mandl and Fine's research, more than 166,000 of them may be treated for it unnecessarily. (CDC PHIL)
Their analysis, published in the Annals of Internal Medicine, makes a strong case for adding biosurveillance into the clinical decision making process. Extrapolating results from the MinuteClinic data to the estimated 10.5 million annual visits patients make to their doctor for strep throat in the U.S., the researchers suggest that by taking such data into account doctors could spare 166,616 patients unnecessary antibiotic treatment and catch 62,537 previously missed cases of strep.
This is not the first time Mandl and Fine have made the case for taking a local view toward diagnosis. The two had previously showed that accounting for local incidence could increase diagnostic accuracy for meningitis, pertussis, and Lyme disease.
“We’re creating a blueprint for feeding population-level data into the clinic that we hope will help bring tighter integration between public health surveillance and clinical care,” Mandl says. “Over time, the broad adoption of tools like electronic medical records will make it much easier to gather this kind of epidemiologic information and disseminate it to clinicians as a way of supplementing their diagnostic toolkit.”







