
With a quick photograph by the pediatrician, a “mystery rash” can be diagnosed remotely.
“Hey, can you take a look at my patient’s rash?”
This question comes up on an almost-weekly basis at Martha Eliot Health Center, the community health center of Boston Children’s Hospital where I see children for primary care. While dermatologic conditions are common in pediatrics, and we, in the primary care setting, often know what to do about them, patients sometimes come in with rashes that don’t look like anything we’ve seen before. In these situations, we wish we could have a trained dermatologist just take a look, but the demand for new dermatology appointments at Boston Children’s is high and wait times for non-urgent clinic visits can be long.
From the dermatologists’ perspective, a large proportion of the patients in their clinic actually don’t actually need to be there—they have common conditions that can be managed in the primary care setting, in the patient’s medical home, in a much more convenient and cost-effective way. Full story »
Telemedicine has the potential to transform healthcare and lower costs. A new Massachusetts law requires insurers to pay for it—but with a potential loophole.

The mandate for broader access to health care in Massachusetts has brought millions of newly insured patients into the system. At the same time, the cost of health care in Massachusetts has continued to rise, and care access issues have emerged.
This past August, Massachusetts Governor Deval Patrick signed a new law that attempts to lower costs by shifting providers away from fee-for-service payment to alternative payment models (APMs) in which they incur more financial risk, and encouraging the development of accountable care organizations (ACOs).
One provision of this law requires insurers to pay providers for services delivered remotely via “telemedicine.” Full story »
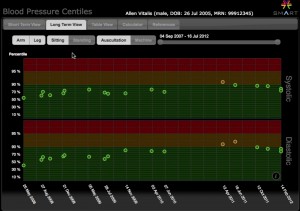
Hypertension is harder to diagnose in children than you think. A new app, which can work with multiple EMR systems, helps doctors interpret a child's blood pressure readings based on age, height, sex and measurement technique, and get the long-range view. (Click to enlarge)
The Affordable Care Act, now the law of the land, mandates free blood pressure screening for children as part of their health care coverage. Yet often hypertension in children is missed, while other children get evaluated and sometimes treated for high blood pressure readings that turn out to have been transient (often induced by kids’ fear of doctors). That has cardiologists like Justin Zachariah, MD, MPH, concerned.
“We’re both overdiagnosing and underdiagnosing hypertension,” says Zachariah, of the Boston Children’s Hospital Preventive Cardiology Clinic. “There must be a problem in the way we’re measuring it.”
Hypertension, or high blood pressure, is being seen more and more often in kids. Its prevalence 15 years ago was about 1 percent; now it’s nearly 5 percent, according to 2011 data from the American Heart Association, likely due to unhealthy diets and lack of exercise. Full story »
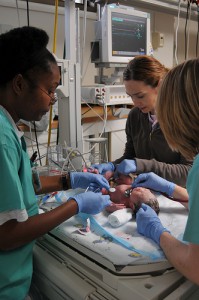
Sepsis, a serious, hard-to-diagnose threat in the NICU, can interfere with a baby's development even when cleared with antibiotics. (Image: Army Medicine/Flickr)
Sepsis, or bacterial infection of the bloodstream, is a grave threat to premature infants in the neonatal intensive care unit (NICU) who have catheters and intravenous lines. Even when antibiotics clear the infection itself, the inflammation that it causes can do just as much damage. Not only can sepsis and the resulting inflammation interfere with fragile preemies’ ability to gain weight, but a growing literature suggests that they can impair brain development.
Preventive measures can now avoid many cases of sepsis, but those that slip through can be hard to detect in newborns.
“Newborns can’t speak, and they have unique immune systems, so they tend not to have fevers or show clinical signs,” explains Ofer Levy, MD, PhD, of the Division of Infectious Diseases at Boston Children’s Hospital. “There may be irregular breathing or increased heart rate, or the baby may be acting a little ‘off,’ but these signs are pretty nonspecific. There’s a tremendous need for better diagnostics in this field.”
Levy and colleagues recently described a mouse model that, for the first time, captures the effects of sepsis on the newborn immune system. They and others have begun using it to identify diagnostic markers and better treatments. Full story »
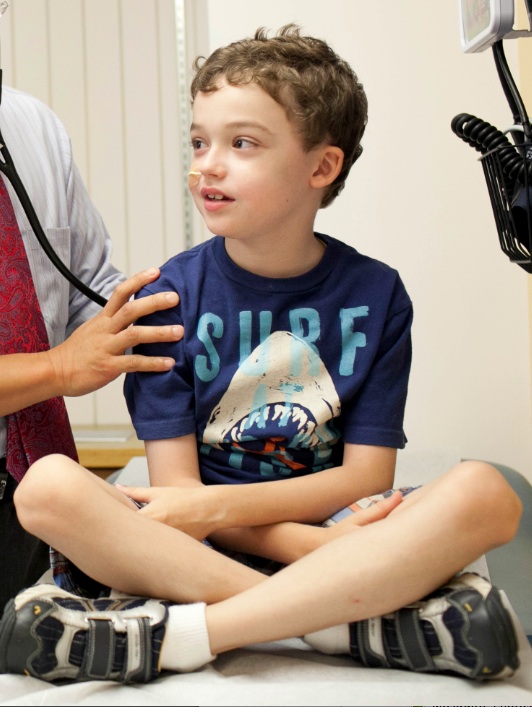
Eosinophilic esophagitis is often misdiagnosed, and seems to be on the rise. (Images: Gretjen Helene Photography)
As an infant, Cameron Ledin sneezed and rubbed his eyes whenever his mother, Kim, nursed him. His growth was slow, and as he got older, it became clear that he had serious feeding problems. When he was old enough for solid foods, he refused to eat. When he was old enough to speak, he complained that eating hurt his stomach.
Over the years, Cameron saw allergy specialists at Boston Children’s Hospital repeatedly, and every visit ended with more confirmed food allergies. By the time he was 7, Cameron could eat only 25 foods, and his pain and symptoms continued. Multiple tests—for airway, pulmonary and upper digestive tract problems—had inconclusive results. Full story »

(Pierre Guinoiseau/Flickr)
People sometimes say that children with autism “march to a different drummer” or “vibrate at a different frequency.” New research analyzing electrical activity in the brain—via electroencephalography, or EEGs—makes it tempting to speculate that these clichés have some truth to them.
EEGs have been around for close to 100 years, and are relatively cheap. But interpretation of these squiggly lines has barely scratched the surface of what they can tell us.
Recent research suggests that EEGs might have a lot to say about how the brain is connected up, and how it processes and integrates information. These messages—if we could properly hear them—might someday help clinicians diagnose autism much earlier than they can now.
The EEG tracks different kinds of rhythms, which show up as waves that oscillate at varying frequencies. Full story »

Mary Elizabeth Stone and her son John, with genetic counselor Meghan Connolly and Pankaj Agrawal, principal investigator of the Gene Discovery Core. (Courtesy ME Stone)
Sequencing a patient’s genome to figure out the exact source of his or her disease isn’t standard operating procedure — yet. But falling sequencing costs and a growing number of successes are starting to bring this approach into the mainstream, helping patients and families while advancing a broader understanding of their diseases.
The Stone family is a case in point. When John and Warren Stone were born, their parents were envisioning life raising identical twins, when suddenly everything changed. On their second day of life, the twins started to have seizures with stiffening of their arms and legs; more alarmingly, they would stop breathing from time to time, requiring a ventilator to help them breathe. Further work-up revealed that both John and Warren were having persistent seizures consistent with Ohtahara syndrome, a rare, debilitating seizure disorder.
Warren died a few weeks later, and the family transferred John’s care to Boston Children’s Hospital. An extensive clinical and genetic work-up here and at several other hospitals involved in his care — including sequencing all the genes known to cause Ohtahara syndrome – identified no cause for John’s unique seizures. Full story »

The Gutenberg press disseminated ideas to a wider society. But in the clinical world, much information is still on "lockdown." (Wikimedia Commons)
The best things in life are free: friends, sunny days, beautiful vistas. Wouldn’t it be nice if knowledge were also free? Historically, libraries promulgated knowledge sharing because it was for the public good. We see this spirit increasingly embraced on the Internet – take the recent announcement of a collaboration between Harvard and MIT to make their courses freely available to users around the world via the edX platform.
But have we made all useful knowledge available in a way that allows for the greatest societal advancement? Not really. According to Ken Mandl, MD, MPH, director of the Intelligent Health Laboratory at the Children’s Hospital Informatics Program (CHIP), one important source of information still on lockdown is clinical trial data. In an article called, “Learning from Hackers: Open-Source Clinical Trials” published this month in Science Translational Medicine (not currently available in full text), Mandl and his coauthors call for making raw, de-identified clinical trial data free to the public. Full story »

Excess brain electrical activity at night can disrupt development -- but if found, may be treatable.
This is the second post in a series about new approaches for seizures and epilepsy. Read the first post here.
When a 2- or 3-year-old child begins losing milestones like language, walking skills and fine motor abilities, or is slow to achieve them, it’s devastating for families. The good news, at least for some children, is that it might be treatable.
Tobias Loddenkemper, MD, a neurologist in the Epilepsy Center at Boston Children’s Hospital, suspected that some children with developmental delay have seizure-like activity in the brain at night. These spikes of electrical activity, referred to medically as sleep-potentiated epileptiform activity, can be readily and inexpensively detected by electroencephalography, or EEG, and readily treated with nighttime anti-seizure drugs.
But likely, no one’s thought of it. “Very few physicians have been looking to see what’s happening at night,” Loddenkemper says.
He and research fellow Iván Sánchez Fernández, MD, with other colleagues, decided to look themselves. Full story »

This comfy wristband can sound an alarm when a child is having a seizure, and can help doctors better time medication dosing.
This is the first post in a series about new approaches for seizures and epilepsy.
Seizures are often hard to track in children with epilepsy, making it difficult for doctors to optimize their treatment. For parents, the greatest worry is that their child will have a life-threatening seizure in the middle of the night or away from home, unable to get help. And what about when that child goes off to college?
“Every parent asks, ‘What can I do to prevent my child from harm?’” says Tobias Loddenkemper, MD, a neurologist in the Epilepsy Program at Boston Children’s Hospital.
Loddenkemper also wanted to better understand his patients’ seizure patterns so he could better time the dosing of their medications. He’s been testing a wristband sensor system, developed by Rosalind Picard, ScD, and colleagues at the MIT Media Lab (Epilepsia, March 20), and thinks it could be part of the solution. Full story »

















