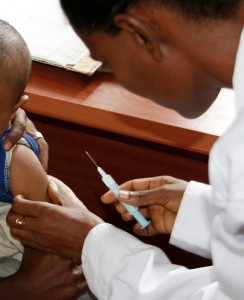
If we could immunize infants at birth, far more could be protected from infections.(DFID-UK Dept for International Development)
Right now, immunizations against most infections begin at 2 months of age. But that leaves newborns at risk for infections like rotavirus, whooping cough and pneumococcus during a highly vulnerable time.
In resource-poor countries, this is a serious problem: Many children see a health care provider only at birth, so may miss their chance to be protected. Worldwide, each year, more than 2 million infants under 6 months old die from infections, especially pneumonia. If we could immunize infants at birth, it would be a huge win for global health.
Unfortunately, though, newborns don’t respond to most vaccines. Their immune systems are too immature—which is why few vaccines for newborns exist.
But back in 2006, a lab led by Ofer Levy, MD, PhD, of the Division of Infectious Diseases at Boston Children’s Hospital, demonstrated that while a newborn’s immune response is weak to nonexistent, one piece rallies robustly: a receptor on white blood cells known as Toll-like receptor 8 (TLR 8). It’s one of 10 known TLRs that are part of our innate immune response—our first, rapid defense against infections.
Also in 2006, as it happens, VentiRx Pharmaceuticals was founded. The Seattle-based company focuses on the development of small-molecule compounds that specifically target TLR8. Rob Hershberg, MD, PhD, the company’s founder and CEO, saw Levy’s publications and recognized a scientist who appreciated TLR8’s appeal. He flew to Boston and began to collaborate with Levy’s lab, providing a panel of synthetic TLR8 stimulators known as benzazepines, already in clinical trials for several cancers with the aim of enhancing anti-tumor immune responses.
“I told him that our compounds would be better than anything he’s worked on,” Hershberg recalls.
Indeed, one of them, VTX-294, proved more potent than anything ever tested. In a study reported last week in the online open-access journal PLoS ONE, it induced an exuberant production of cytokines (chemicals that rally the immune response) in newborns’ white blood cells, at levels at least 10-fold that of the best activator of TLR8 known previously.
“VTX-294 not only produced an equal cytokine response in newborns, it was sometimes actually more effective in newborns than adults,” Levy says.
The compound also triggered production of so-called co-stimulatory molecules that enhance immune responses. Better still, even very small amounts of VTX-294 strongly activated antigen-presenting cells, specialized white blood cells that engulf pathogens and display bits of them to the long-term-memory part of the immune system, creating a memory of the invader. Activating these cells is critical for a vaccine’s effectiveness.
“This one receptor seems to lead to more adult-like responses—immediate, short-term responses that are more appropriate for fighting infections,” says David Dowling, PhD, co-first author on the study.
Could VTX-294 make vaccines effective right at birth? Dowling and Levy hope so. With encouraging results in newborn infants’ cells, they now hope to formulate the compound, or a similar TLR8 stimulator, and test it as a vaccine adjuvant in newborn monkeys—a model in which the lab has expertise, and whose responses to TLR8 closely resemble humans’.
“We’re excited about the benzazepines because they are already in the clinical pipeline. That advances the potential for using them in a clinical study in human newborns, once they have been proven safe in animal studies.”
For further background on the Levy lab’s work, see this blog post from 2010.








