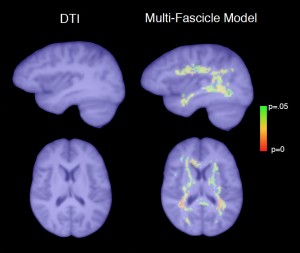
A new MRI computational technology (above right) captures differences in water diffusion in the brain across a population of children with autism as compared with controls. This non-directional, “isotropic” diffusion pattern, not evident with conventional diffusion tensor imaging (DTI), may be an indicator of brain inflammation.
Diffusion tensor imaging (DTI), a form of magnetic resonance imaging, has become popular in neuroscience. By analyzing the direction of water diffusion in the brain, it can reveal the organization of bundles of nerve fibers, or axons, and how they connect—providing insight on conditions such as autism.
But conventional DTI has its limits. For example, when fibers cross, DTI can’t accurately analyze the signal: the different directions of water flow effectively cancel each other out. Given that an estimated 60 to 90 percent of voxels (cubic-millimeter sections of brain tissue) contain more than one fiber bundle, this isn’t a minor problem. In addition, conventional DTI can’t interpret water flow that lacks directionality, such as that within the brain’s abundant glial cells or the freely diffusing water that results from inflammation—so misses part of the story.
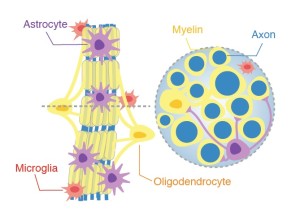
A slice of a fiber bundle contains not only nerve fibers (shown in blue), but also glial cells including oligodendrocytes, astrocytes and microglia. The presence of these cells can be inferred through mathematical modeling.
In a paper published last month in IEEE Transactions on Medical Imaging, researchers detail a technical breakthrough: a standardized mathematical framework that is able to glean more information from a scan that could shed further light on brain abnormalities and can potentially be used by any research center.
“We can now look simultaneously at patterns of water diffusion inside the fibers and unstructured patterns outside the fibers, like cars driving off-road,” explains Maxime Taquet, PhD, first author on the paper and a research fellow in Boston Children’s Hospital’s Computational Radiology Laboratory. “We also can characterize the connections (small roads versus highways), visualize and analyze crossing pathways and detect abnormalities along the tracts.”
“This work takes research on fiber structures to the next level,” says Boston Children’s neurologist Jurriaan Peters, MD, one of the co-authors on the paper. “The current diffusion tensor model just tells us the main direction of axons. We can’t tell whether there are other cell types there. The novel model also allows for doing group comparisons—critical to better understanding diseases.”
Moreover, adds Taquet, image acquisition time with the new method can be shaved to as little as six minutes, making this kind of detailed brain imaging more feasible for research and clinical use.
The researchers hope the new technology will aid in understanding conditions that may involve brain inflammation, such as autism. In the paper, Taquet and senior investigator Simon Warfield, PhD, of the Computational Radiology Laboratory, report preliminary results of imaging the brains of patients with tuberous sclerosis complex (TSC), a genetic condition that includes autism in about half of patients.
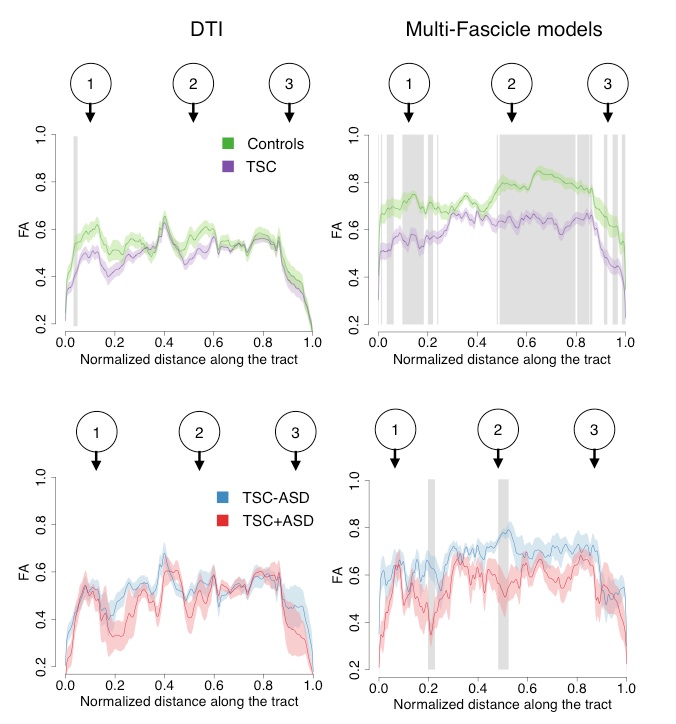
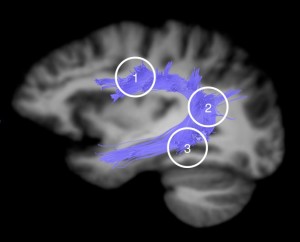 The image at left, for example, shows nerve tracts in the dorsal language circuit of a healthy brain. Below is the team’s analysis of TSC patients using the new mathematical model. The numbers 1, 2, 3 over each column match the brain locations in the scan. The top two graphs compare tracts in 38 TSC patients versus 24 controls. The vertical grey lines in the right-hand graph indicate places along the tracts where the TSC patients show significantly less directionality of water diffusion than controls, possibly reflecting damage to the axons or to the myelin sheath encasing the nerve fibers. Similarly, the bottom two graphs TSC patients with and without autism. As indicated by the grey lines, the group differences were more pronounced and robust with the new “multi-fascicle” model than with conventional DTI.
The image at left, for example, shows nerve tracts in the dorsal language circuit of a healthy brain. Below is the team’s analysis of TSC patients using the new mathematical model. The numbers 1, 2, 3 over each column match the brain locations in the scan. The top two graphs compare tracts in 38 TSC patients versus 24 controls. The vertical grey lines in the right-hand graph indicate places along the tracts where the TSC patients show significantly less directionality of water diffusion than controls, possibly reflecting damage to the axons or to the myelin sheath encasing the nerve fibers. Similarly, the bottom two graphs TSC patients with and without autism. As indicated by the grey lines, the group differences were more pronounced and robust with the new “multi-fascicle” model than with conventional DTI.
Warfield and study co-author Mustafa Sahin, MD, PhD, are now recruiting children age 5 to 10 years for a much larger five-year study looking at MRI biomarkers in patients with TSC and/or an autism spectrum disorder. The study will apply the multi-fascicle model, as well as other MRI measures that could help in diagnosing autism earlier. With further refinement and validation, Peters also sees potential applications in other brain disorders with an inflammatory component, such as traumatic brain injury and some forms of epilepsy.
“It’s too early to call these findings biomarkers,” cautions Peters, “but that’s something we would like to investigate.”
Families of both affected and healthy children who are interested in participating in the study can inquire directly on the Computational Radiology Laboratory’s recruitment form.