
In a one-two-three punch, a rapid screen in zebrafish can quickly identify a short list of drug candidates to test in mice and in patient-derived cells.
But what really excites Zon, director of the Stem Cell research program at Boston Children’s Hospital, is the power of the chemical screening platform he and his colleagues used. Described last week in the journal Cell, it found a cocktail of three compounds that induced human muscle cells to grow—in just a matter of weeks. Zon believes it could fast-track drug discovery for multiple disorders.
The Zon Lab has already made a name for itself with its zebrafish drug-screening platform, using it to identify a drug that boosts production of blood stem cells. Originally developed to treat stomach ulcers, that drug is now being developed under the name ProHema to help patients receiving cord blood transplants recover their immune function more quickly. It is now in a Phase II clinical trial, sponsored by Fate Therapeutics.
Zebrafish chemical screening on steroids
Zon’s original technique involved loading tiny, fast-growing zebrafish into 96-well plates, adding a different chemical to each well, and then examining the fish in the lab to see which ones displayed the desired effect (in the above case, more blood cells).
But the process involved laborious and time-consuming biochemistry. Zon and colleagues wanted something faster. So, in their first step, they placed tiny zebrafish blastomeres—cells from very early stage embryos—into 384-well culture dishes. They also genetically modified the blastomeres, so any newly created muscle progenitor cells would show up in fluorescent green and muscle fibers in red.
“Automated imagers can take a picture to assay all the 384 wells within a matter of a week, compared with several months with our earlier technique,” Zon explains.
The colors are readily visible in the developing embryos (which, unlike adult zebrafish, are see-through), as in this young fish:
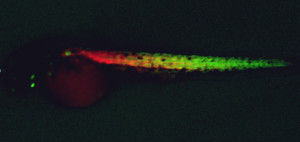
Within a week, this rapid culture system enabled them to narrow 2,400 different chemicals down to just six.
Validation in mice and human cells
For the second step, the Zon Lab collaborated with Amy Wagers, PhD, and C. Ronald Kahn, MD, of the Joslin Diabetes Center, to test the six compounds in a mouse model of Duchenne muscular dystrophy. One compound, forskolin, increased engraftment of progenitors into the muscles of the mice, thereby increasing muscle mass. (Interestingly, forskolin has been used since ancient times for a variety of disorders and is sold as a dietary supplement; Dr. Oz has hailed its metabolism-boosting properties.)
In the final step, Zon, Wagers, Kahn and colleagues took skin cells from patients with Duchenne muscular dystrophy and converted them genetically into induced pluripotent stem cells (iPS cells), a technique increasingly used to model disease in a dish. “Many muscle diseases could not be adequately modeled in iPS cells in the past,” notes Zon. “No one’s been able to get iPS cells to form skeletal muscle.”
It turned out that a cocktail of forskolin and two other small molecules could reprogram iPS cells into muscle cells, and that these cells could successfully engraft in mice. Zon’s next goal is to transplant them into patients in a clinical trial he expects to be developed in several years. The first trial might focus on increasing muscle mass in a specific anatomic location, but for a condition like Duchenne muscular dystrophy, Zon envisions a series of local injections in different parts of the body.
Broader applications
Zon believes that the rapid zebrafish screening platform—for which he’s filed a patent—will greatly speed up therapeutic development when combined with patient-specific iPS cells, allowing scientists to quickly vet large numbers of compounds and possible culture conditions.
“We’ve created a very fast system to find what chemicals you need,” he says. “Because it’s so fast, we don’t need a hypothesis to do an experiment—you can just do the screen, find the result and see what warrants pursuing.”
Industry representatives interested in the zebrafish platform can read more here or contact licensing manager [email protected].






