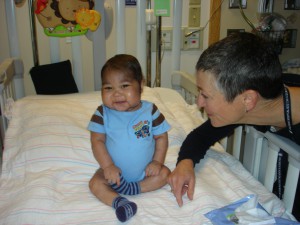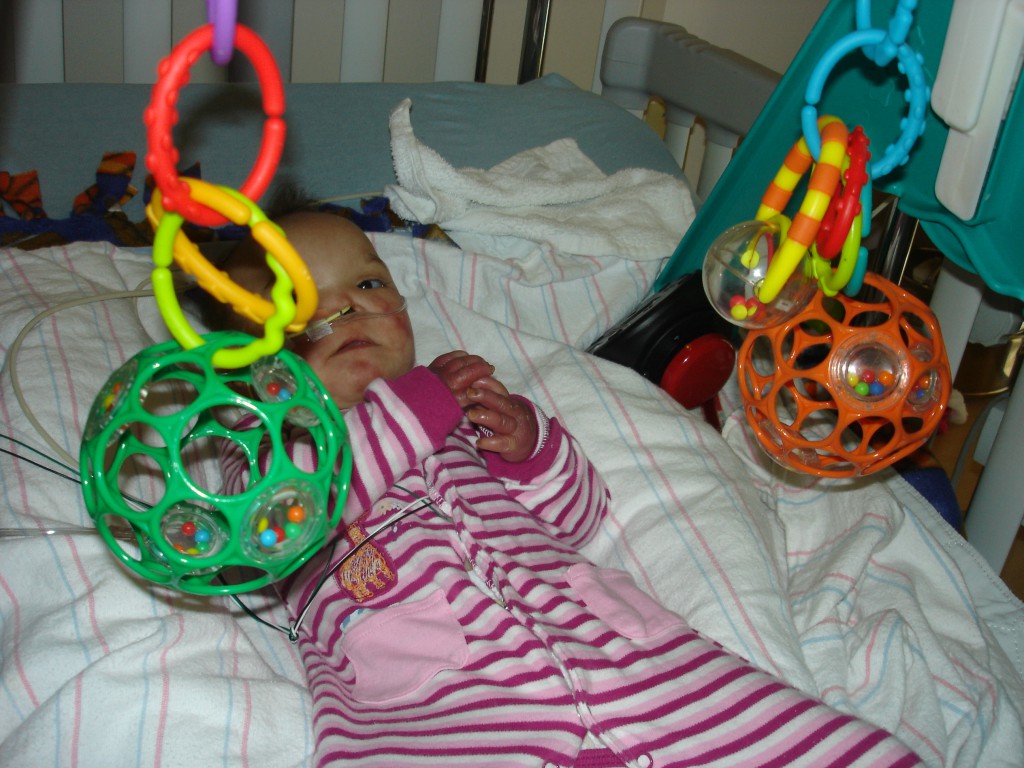
Afraa Bakhit, from the Middle East, is among the hospital's most complicated patients. Her disorder is unknown.
This is the first post of a two-part series on children with complex medical needs. Details on some patients have been changed for privacy reasons.
This morning, as every morning, the Complex Care Service (CCS) team huddles in a tiny office deep inside Boston Children’s Hospital. They have 14 patients to discuss, each with a mix of problems that involve multiple clinical departments. Many of them are repeat visitors.
The team begins tackling each case in decreasing order of difficulty. “It seems to be the best way to prioritize the patients with the most immediate needs,” says Mindy Morin, MD, MBA, who’s the attending physician this week. Also on the team are two nurse practitioners, a clinical nurse educator and two resident physicians.
Two-year-old Afraa Bakhit from Dubai tops the list for the sheer number of departments consulting on her case: Genetics, Cardiology, Immunology, Infectious Disease, Rheumatology, Pulmonology, Anesthesia and now a specialist from the Vascular Anomalies Center. Her unknown disorder has caused her hands and feet to turn blue from poor circulation, resulting from some mysterious problem in her blood vessels. It also affects her heart and lungs, and she’s lost part of her nose, through which she’s being tube-fed a high-calorie diet.
Afraa first went to Germany for care, then back to Dubai, and now she’s here. Indeed, Boston Children’s has become a hub for Middle East families with genetic disorders. “No one knows what she has,” Morin says.
Perplexing as Afraa’s case is, the CCS can do only limited diagnostic testing. “We have to prioritize blood draws because she also has chronic anemia,” Morin explains. “We need to focus on tests that are going to impact her immediate care.”
Long-term care needs

The Complex Care Service team huddles before formal morning rounds. (L-R: Jen Tucker, RN; Sarah Wells, CCS Nurse Specialist; Mindy Morin, MD, CCS attending physician; Sarah Packard, MD, pediatric resident.)
High on the team’s list is a teen with a brain injury that has caused spasticity in her arms and legs, incontinence and chronic lung disease, a complication of impaired swallowing. She’s just had surgery to implant a baclofen pump to ease her spasticity. “Today is going to be a painful day for her,” Morin reminds the team. They discuss the day’s pain management and her history of post-traumatic stress disorder.
They next turn to a neurologically impaired young woman with an overactive bladder. She is paralyzed from the waist down, and came to the emergency room last night with a raging urinary tract infection.Her family is supposed to make sure she changes her catheters at home and periodically irrigates her bladder, but the team wonders whether these things are happening often enough.
“There’s something going on,” she says. “Honestly, her UTI could be treated outpatient, but we thought, ‘let’s bring her in and try to get to the bottom of why she keeps returning to the hospital.’”
It’s not unusual for Boston Children’s to continue seeing patients into adulthood, especially if they have genetic or congenital disorders where pediatric specialists have expertise. But sometimes patients outgrow the hospital’s ability to care for them. Another woman needs surgery for a complication of a spina bifida repair she had as a child. It’s an adult operation that the surgeons at Boston Children’s don’t customarily perform, so she’s waiting for a bed to open up at another Boston hospital. Morin will try to move her up the list.
Opposing incentives
Carlos, 20 months old, arrived at Boston Children’s in July from Puerto Rico, emaciated and debilitated. His case is happier than most. A comprehensive work-up has found the cause for his failure to thrive: colitis, an autoimmune bowel disorder that’s been reversed by giving him anti-TNF alpha antibodies. “This was an amazing save,” Morin says. The team is prepping a smiling, plumper Carlos for discharge and planning his future care with specialists in Puerto Rico.
The team is perplexed by the case of a boy with cerebral palsy and seizures, who has just been readmitted with aspiration pneumonia. It’s unclear why this happened—he looked great when discharged just four days earlier, “like a rose,” reports Clinical Nurse Specialist Sarah Wells.
Tracy Allen, one of the team’s nurse practitioners, wonders about care at home, which should include regular suctioning of mucus, a vibrating vest to break up thick lung secretions, specially compounded medications and more.
Such care is difficult to keep up with. Families often have to maintain miniature ICUs in their homes to keep their children alive. Many parents have to quit their jobs, and marriages often dissolve under the stress.
“Families need more support at home,” Morin says. “As a physician, my readmission rate is followed, and if a patient is readmitted within 30 days, insurance can decide not to pay. On the flip side, our patients’ length of stay is also tracked, so we have two opposing incentives. The rules work for general patients, but not complex patients.”

Genetic and congenital disorders--and even child abuse or severe infections--can lead to lifelong complex care needs.
The team turns to a little boy who contracted a virulent infection. Where it came from is unclear, but it landed him in the intensive care unit three months ago with end-stage kidney disease, a bowel infarction, stroke and cardiac arrest.
“Now he’s stable, but it took a long time to get to that point, and he has multiple chronic medical problems,” says Morin. Allen has created a detailed binder with his medical information and what he likes and doesn’t like, for the rehab facility where he’ll go next.
A toddler with a chronic, unknown metabolic disorder was sent here by a long-term care facility. He has a tendency to get very sick very quickly, and the care facility is refusing to take him back, in part because his family does not want a Do Not Resuscitate/Do Not Intubate order. “That makes it hard to place him,” says Morin. “The facility feels he is too unstable to care for safely, but home just isn’t an option for this family.”
After discussing a half-dozen other cases, the meeting ends. “Strong work!” Morin tells the team. “That was a challenging list we just went through.”
In our next post, we follow the care team during morning rounds and explore how the current health care structure jeopardizes the care of children with complex care needs.