
Colombian twins Miranda and Olivia Agudelo (with their parents) were the first patients in a clinical trial aimed at making the bone marrow transplant process less toxic.
One thing that most people don’t realize about stem cell transplants (also called bone marrow or hematopoietic stem cell transplants) is that for patients, the transplant itself is probably the easiest part of the process. The grueling part is the preparation for a transplant, called conditioning.
There’s been a lot done at Dana-Farber/Children’s Hospital Cancer Center (DF/CHCC) and elsewhere to make conditioning less toxic. With a new clinical trial in a rare genetic syndrome called dyskeratosis congenita (DC), doctors at DF/CHCC are taking an even bolder step.
Stem cell transplants can be lifesavers for patients with conditions like relapsed leukemia or bone marrow failure syndromes like aplastic anemia or Fanconi anemia, where their own stem cells are the cause of the problem. But whenever blood stem cells come from a donor (a so-called allogeneic transplant), patients have had to be conditioned with radiation and chemotherapy to wipe out their own supply. This can cause a lot of collateral damage to other organs, a real concern given the weakened state many patients are in by the time they get to the point of a transplant.
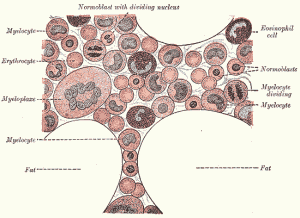
Bone marrow stem cells produce every kind of blood and immune cell in the body. (From Gray's Anatomy of the Human Body 1918/Wikimedia Commons)
“Because the conditioning process is so difficult, we usually only give stem cell transplants to treat life-threatening disease,” says Suneet Agarwal, MD, PhD, an expert in bone marrow failure syndromes with DF/CHCC’s Stem Cell Transplantation Program who studies DC. “Reducing or eliminating the toxicity would let us offer stem cell transplantation for many more children and adults with blood or immune diseases.”
From reduced intensity to no intensity
Many centers, including DF/CHCC, have developed “reduced intensity” conditioning regimens, ones that rely less on chemotherapy and radiation and more on suppressing patients’ immune responses. DF/CHCC now uses a reduced intensity regimen as the standard regimen for all patients with bone marrow failure.
But Agarwal and colleagues want to do more. They want to eliminate chemotherapy and radiation entirely, and go with immunosuppression only. In theory this would keep the patient’s immune system quiet while the transplanted stem cells move in (also called engraftment) and push the dysfunctional stem cells out. But with no chemotherapy or radiation involved, there’s far less toxicity from the conditioning.
Reducing or eliminating the toxicity of conditioning could make stem cell transplantation an option for many more children and adults with blood or immune diseases.
Agarwal is trying this new immunosuppression-only conditioning approach in a clinical trial in children with DC. About 80 percent of them need stem cell transplants before age 30 due to bone marrow failure, though carrying out those transplants is especially difficult.
“There’s been a general sense over the last decade that children with DC have a harder time than usual with transplant conditioning,” Agarwal notes. “We think it’s because the mutations that cause the disease cause other organ problems that make the toxicity worse.”
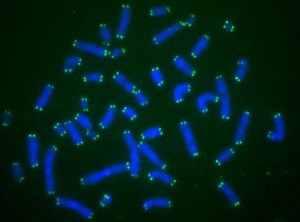
Telomeres (the green dots capping the blue chromosomes) get shorter as we get older. In children with dyskeratosis congenita, genetic mutations make them get too short too quickly.
Those very mutations, however, make DC an attractive target for trying immunosuppression-only conditioning. The cells of children with DC have a problem with their telomeres—the caps on the ends of cells’ chromosomes. In all of us, the telomeres get shorter as we age. Cells have mechanisms for keeping the telomeres from getting too short too quickly, but in DC those mechanisms don’t work.
“Because the telomeres get really short, the bone marrow stem cells in a person with DC don’t divide very well,” Agarwal explains. “Which may mean they can’t produce robust immune responses.” Which, in turn, means that patients with DC can’t mount a strong immune attack against transplanted stem cells.
Promising results
Agarwal’s DC trial is still in its early stages, but to date he and Leslie Lehmann, MD, medical director of DF/CHCC’s stem cell transplant program, have treated three children, two of them twins from Colombia who came to DF/CHCC this past summer just for the trial.
So far the results are promising. “All three patients had very few problems during conditioning, and their transplanted cells engrafted more quickly than usual,” he says. “The trial has a 15-year follow-up period because we want to track their long-term outcomes, but in the short term things look very good.”
All of which suggests that this nontoxic approach to conditioning could be a winner. “Our biggest concerns going into the trial were whether the patients’ transplanted cells would still be able to engraft, whether the patients would still need transfusions for their bone marrow failure and whether there would be major complications,” Agarwal says. “The answers have been yes, no and no, which is what we’d hoped for. Can they sustain their grafts in the long term? That we don’t know yet, but we’re hopeful.”
To learn more about the bone marrow transplant trial for dyskeratosis congenita, read the story of Olivia and Miranda Agudelo, the first children to join the trial, on Thriving or visit the trial information page.








