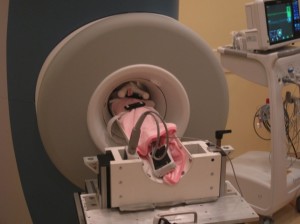
A 4.2-lb baby girl in the new 1.5 Tesla MRI magnet, designed for use in the NICU. (Images courtesy of Cincinnati Children’s Hospital Medical Center)
Charles Dumoulin, PhD, is the director of the Imaging Research Center at Cincinnati Children’s Hospital Medical Center (CCHMC) and a professor of pediatric radiology at University of Cincinnati College of Medicine. He led the team of scientists and engineers from CCHMC’s Imaging Research Center who won the Clinical Innovation Award at Boston Children’s Hospital’s National Innovation Pediatric Summit + Awards in September.
Experience suggests that magnetic resonance imaging (MRI) and advanced MR techniques such as spectroscopy and diffusion imaging offer substantial benefits when diagnosing problems in premature babies. However, today’s MR systems poses significant logistical barriers to imaging these infants. We have been working to change that.
MRI provides an unparalleled ability to visualize anatomy without the hazards of ionizing radiation. Yet premature and sick babies in neonatal intensive care units (NICUs) are usually too delicate to leave the unit. The few babies who receive MRI today must be accompanied by NICU staff during transport to and from the Radiology Department. This process is often a multi-hour ordeal and reduces the staff available to care for other babies in the NICU. Moreover, infants must be imaged in an adult-sized MRI scanner Full story »
 Wrapping up the National Pediatric Innovation Summit + Awards on Sept. 27, emcee Bruce Zetter, PhD, who runs a lab in Boston Children’s Vascular Biology program, remarked, “I thought I was going to learn about technology. What I learned about was communication.”
Wrapping up the National Pediatric Innovation Summit + Awards on Sept. 27, emcee Bruce Zetter, PhD, who runs a lab in Boston Children’s Vascular Biology program, remarked, “I thought I was going to learn about technology. What I learned about was communication.”
Surgeon, writer and public health researcher Atul Gawande, MD, MPH, laid bare this often overlooked element of medicine in his closing keynote. He eloquently made the point that communication—and more specifically systems—is where innovation is most needed and where it can have the most impact.
“We have emerged from the century of the molecule to the century of the system,” Gawande said.
Right now, these systems are broken, seemingly everywhere. Gawande recounted the sad tale of Duane Smith, a patient who survived a severe car crash that ruptured his spleen, only to lose his fingers, toes, nose and job from an ordinary strep infection. Full story »
 At the start of today’s National Pediatric Innovation Summit + Awards 2013 panel on patient engagement, healthcare journalist Carey Goldberg offered up a personal anecdote about engagement— or the lack of it—in medical care:
At the start of today’s National Pediatric Innovation Summit + Awards 2013 panel on patient engagement, healthcare journalist Carey Goldberg offered up a personal anecdote about engagement— or the lack of it—in medical care:
“I was having a minor dermatological procedure, and right before it started, I said to the doctor, ‘This really is a good idea to get this done, right?’ And she said, ‘No, actually, you don’t really need to get it done.’ And I didn’t stop the procedure. And I realized that I embodied the problem of patient engagement. It is a piece of [the health care] puzzle.”
Goldberg’s story framed a discussion that ranged from outcomes measurement to data access, from healthcare incentives to care coordination—all centered on one overriding question: How do we encourage patients to become more engaged in their own medical care?
And given the number of topics that were covered, it’s clear how complex a question that is. It’s one that engages multiple stakeholders—patients and their doctors for starters, but also insurers, policymakers and regulators, health care systems and more. Full story »
 There’s been an explosion of scientific research in autism—from mouse models of genetic syndromes involving autism to culturing neurons from stem cells derived from patients’ skin to tracking EEG patterns in infants whose brothers or sisters have autism.
There’s been an explosion of scientific research in autism—from mouse models of genetic syndromes involving autism to culturing neurons from stem cells derived from patients’ skin to tracking EEG patterns in infants whose brothers or sisters have autism.
So I expected yesterday’s panel on Piecing Together the Autism Puzzle, part of Boston Children’s National Pediatric Innovation Summit, to be about the science. I changed my seat just before it started, so I could better view the slides.
Instead, the conversation turned to the insurance, public health and social justice aspects of autism. Take, for example, the rising incidence of autism, which the CDC places at 1 in 88 (and 1 in 54 in boys). Panelist Ami Klin, PhD, director of the Marcus Autism Center at Children’s Healthcare of Atlanta, noted that between the CDC’s 2002 and 2008 reports on autism, there was close to a 101 percent increase in autism prevalence in Hispanics and a 96 percent increase in blacks.
Thousands of children didn’t suddenly develop autism in a six-year span; rather, more were diagnosed with autism as awareness of the disease increased. Even so, diagnoses often don’t occur until a child is 3 to 5 year old, and only 2.5 percent of diagnostic assessments of autism are using the field’s best standardized tools. While multiple diagnostic tests are being researched—like EEGs or blood tests looking at gene expression—they’re still experimental. Full story »
 Early-stage researchers face a stark economic reality: decreasing available dollars. To address this barrier, a panel of experts at Boston Children’s Hospital’s National Pediatric Innovation Summit + Awards 2013 discussed the shifting of funding from venture capitalists to larger medical device, informatics and pharmaceutical companies.
Early-stage researchers face a stark economic reality: decreasing available dollars. To address this barrier, a panel of experts at Boston Children’s Hospital’s National Pediatric Innovation Summit + Awards 2013 discussed the shifting of funding from venture capitalists to larger medical device, informatics and pharmaceutical companies.
Alan Crane, general partner at venture capital (VC) firm Polaris Partners, said it is a very difficult time for early-stage life sciences innovation, especially with respect to resource generation. “There were periods when innovation was stronger,” he said. “In 2000, there were 1,000 VC firms, now there are 350. Also, the size of the funds has decreased substantially, particularly for early-stage life sciences. While some biotech firms are going public, this trend hasn’t trickled to the earlier stages.”
To garner funding, Crane said, researchers need a proof of concept—for a clinical model and a business model. This proof of concept will vary based on the product or the nature of the innovation. Full story »

Vertex Pharmaceuticals CEO Jeffrey Leiden, MD, PhD, at Boston Children’s Hospital’s National Pediatric Innovation Summit + Awards 2013. (Courtesy Vertex Pharmaceuticals)
“I can’t imagine a better time to have an innovation summit in pediatric medicine. We’ve reached a tipping point in pediatrics medicine with scientific innovations converging to completely change the way we think about and treat pediatric disease,” Jeffrey Leiden, MD, PhD, president and CEO of Vertex, shared during the opening keynote at Boston Children’s Hospital’s National Pediatric Innovation Summit + Awards 2013. Full story »
 Over the past few months, the Vector team has been collecting definitions from varied thought leaders—inside and outside Boston Children’s—and the responses have reflected the varied nature of their respective fields. In this series, the term has been called “clichéd” at one extreme to “necessary” for the evolution of care delivery at the other. This week’s respondents range from former FDA leaders to informatics experts to critical care specialists to bioengineers. Follow our continuing coverage of innovative efforts through this week’s National Pediatric Innovation Summit + Awards.
Over the past few months, the Vector team has been collecting definitions from varied thought leaders—inside and outside Boston Children’s—and the responses have reflected the varied nature of their respective fields. In this series, the term has been called “clichéd” at one extreme to “necessary” for the evolution of care delivery at the other. This week’s respondents range from former FDA leaders to informatics experts to critical care specialists to bioengineers. Follow our continuing coverage of innovative efforts through this week’s National Pediatric Innovation Summit + Awards.
Innovation is the belief that we have an obligation to move the world forward through positive and lasting change, leaving it better than we found it. —Jeffrey P. Burns, MD, MPH, Chief of Critical Care Medicine; Director, Medical/Surgical Intensive Care Unit, Boston Children’s Hospital
Innovation is the process of significantly and meaningfully changing the way things are done, operate or perform. Most people think of innovation in terms of the individual developing a novel idea and inspiring or causing change. I think what is often overlooked is the power of a large organization to provide meaningful innovation on a broad scale—it’s not just the single individual that can innovate. Great examples of this are the Apollo mission to the moon, Google, the Internet, the Boeing 747 or, in health care, the development of advanced medical devices. The key to innovation, either as an individual or as a large organization, is to provide transformative change. —Robert “Chip” Hance, CEO of Creganna-Tactx Medical; former Entrepreneur-in-Residence at the FDA Full story »
 In Part 1 last week, Vector took a look at digital health apps, telemedicine, genomics, phenomics and new behavioral diagnostics as transformative trends in pediatrics. This week, we complete our list. These posts will also appear as an article in the fall issue of Children’s Hospitals Today magazine.
In Part 1 last week, Vector took a look at digital health apps, telemedicine, genomics, phenomics and new behavioral diagnostics as transformative trends in pediatrics. This week, we complete our list. These posts will also appear as an article in the fall issue of Children’s Hospitals Today magazine.
6. New pharma research and development (R&D) models
Academic medical centers have always worked with the pharmaceutical industry but never so closely as now. In the old model, industry drove therapeutic development. A company might fund an academic project or supply reagents, but the relationship generally ended with the project (and publication of a paper).
Now, with drug pipelines drying up and R&D costs rising, Big Pharma is under pressure to change. New industry-academia collaborations are forging creative partnerships, altering how both parties do business. The new models are allowing hospital researchers to do what they’ve never done before: take the lead in R&D. Full story »

An early innovation: Specially bred cows graze in front of Boston Children’s Hospital in 1919, providing safe, tuberculosis-free milk for patients.
Clinicians wanting to develop new devices and treatments for children face formidable barriers: regulators’ need to protect the most vulnerable coupled with a lack of commercial interest. But determined innovators do have options, including creative funding sources, says
Thomas Krummel, MD, director of surgical innovation at Stanford Medical School.
“Technology developed specifically for children has been a low priority,” Krummel began at a two-part talk at Boston Children’s Hospital this summer (read our coverage of the other part). “The FDA barriers are incredibly high, and ultimately, investors just demand returns that pediatric markets won’t necessarily deliver.”
As Krummel detailed, the FDA barriers are there for a reason: a past history of ethical abuses in human subjects research. In 1966, physician Henry Beecher, MD, exposed many examples in The New England Journal of Medicine, such as withholding effective treatment for the sake of research, proceeding with a treatment despite recognized hazards, or failing to disclose risk to patients. Institutional Review Boards (IRBs) arose in the mid-1970s to protect research subjects—protections that are especially strict when that research is done in children.
But there’s also a deep-seated reluctance to break with the status quo. Full story »
 Since our “trends” posts at the top of the year are among our most viewed, Vector took time out this summer to take an interim snapshot of pediatric medicine’s cutting edge. Here we present, in no particular order, our first five picks. Check back next Friday for Part 2. If you want more, there’s still time to register for our National Pediatric Innovation Summit + Awards (September 26-27). The posts will also appear as an article in the fall issue of Children’s Hospitals Today magazine.
Since our “trends” posts at the top of the year are among our most viewed, Vector took time out this summer to take an interim snapshot of pediatric medicine’s cutting edge. Here we present, in no particular order, our first five picks. Check back next Friday for Part 2. If you want more, there’s still time to register for our National Pediatric Innovation Summit + Awards (September 26-27). The posts will also appear as an article in the fall issue of Children’s Hospitals Today magazine.
1. Digital health apps 2.0
The electronic revolution in health care continues. According to recent surveys, more than 90 percent of physicians have smartphones and more than 60 percent are using tablet devices like iPads for professional purposes. Dr. Eric Topol and others think these digital tools are the future of medicine.
Mobile apps keep proliferating, adding more and more features: high-quality image capture, voice-to-text capabilities and gaming techniques to motivate adherence, as well as sensors that gather physiologic data, like glucose levels and heart rate. Consumers are tracking and sharing data themselves, saving time in the clinic and helping physicians monitor their symptoms. Through the much-hyped Google Glass, it won’t be long before doctors can seamlessly call up patient data, look up a drug dosage and get decision support during a clinical visit without using a hand-held device.
One limiting factor in this “Wild West” scenario is the FDA’s ability to keep up with digital advances from a regulatory standpoint. Full story »
















