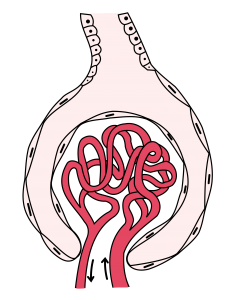
Focal segmental glomerulosclerosis (FSGS) is the second leading cause of kidney failure in children. It ruthlessly attacks the kidney’s filtering system: The glomeruli, tiny clusters of capillaries within each nephron that filter toxins from the blood, scar, harden and stop working. Patients are forced onto chronic dialysis and, all too often, need a kidney transplant.
“To make matters worse, many patients have recurrence of the disease soon after transplant,” says William Harmon, MD, chief of Children’s Division of Nephrology. “First it ruins your native kidney, then it can return instantly in the transplant and ruin that also.” Amazingly, this can sometimes happen within hours of transplantation.
Genetic sleuthing by researchers at Children’s and Brigham and Women’s Hospital recently uncovered one important cause of FSGS – a defect in the gene for INF2. Biologically, this makes some sense: INF2 seems to help regulate the structure of podocytes, the cells that do the filtering. When it’s defective, podocyte structure and function are disrupted, the researchers believe.
Children’s and the Brigham recently entered a licensing agreement with Athena Diagnostics, and the company now has an INF2 blood test on the market to help clinicians identify the genetic cause of a patient’s kidney failure and determine his or her clinical risk (the original research, reported in Nature Genetics late last year, detected 9 separate mutations of the gene).
The market is a sizeable one: According to NephCure, which helped fund the research, 26 million Americans suffer from chronic kidney disease, of which FSGS is one of the most common forms.
Beyond diagnostic testing, it’s hoped that the INF2 discovery, and what it reveals about the biology of a normal kidney, will also translate into better treatments for FSGS – a disease that currently leaves patients with no good options.